The principal objective of a Central Sterile Supplies Department (CSSD) in reprocessing reusable medical devices is to ensure that any contamination on the device from the previous patient is fully removed and is ready to be used on a subsequent patient safely. There are several challenges that make the reprocessing of medical devices difficult.
They are difficult to remove from medical devices using conventional CSSD decontamination processes.
– 5 Stages.
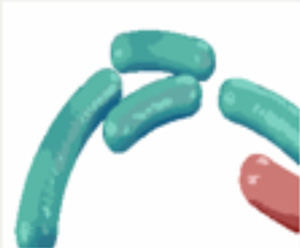
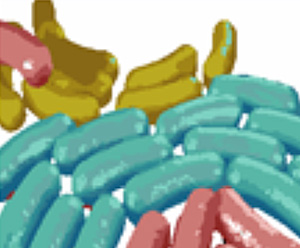

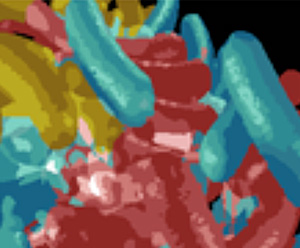


Reference: Journal of Hospital Infection (2004) 58, 224-2
In the paper by Pajkos, Vickery and Cossart and published in the Journal of Hospital Infection clear evidence was presented of the existence of biological deposits in all endoscopes and bacterial films in five out of the thirteen endoscopes examined. Routine cleaning procedures did not remove biofilms and can be a source of infection to subsequent patients.
Intragenic transmission of the CJD agent has been reported in over 500 patients. These cases have been linked to the use of contaminated human growth hormone, dura mater and corneal grafts, or neurosurgical equipment. Of the six cases linked to the use of contaminated equipment, four were associated with neurosurgical instruments, and two with stereotactic EEG depth electrodes.
Infection Control I Creutzfeldt-Jakob Disease, Centre for Disease and Control Prevention
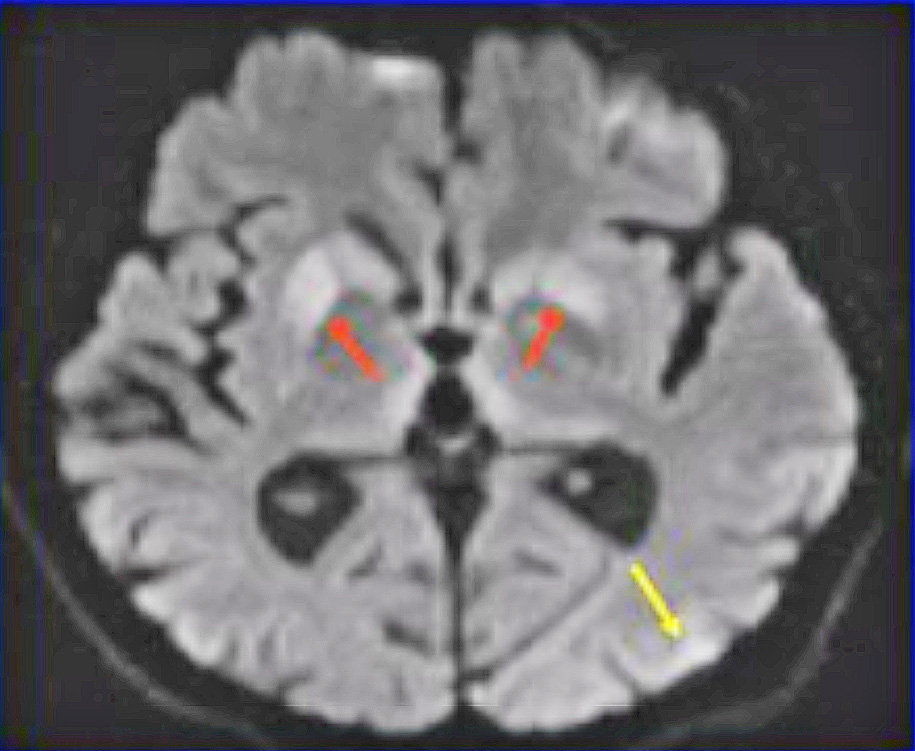
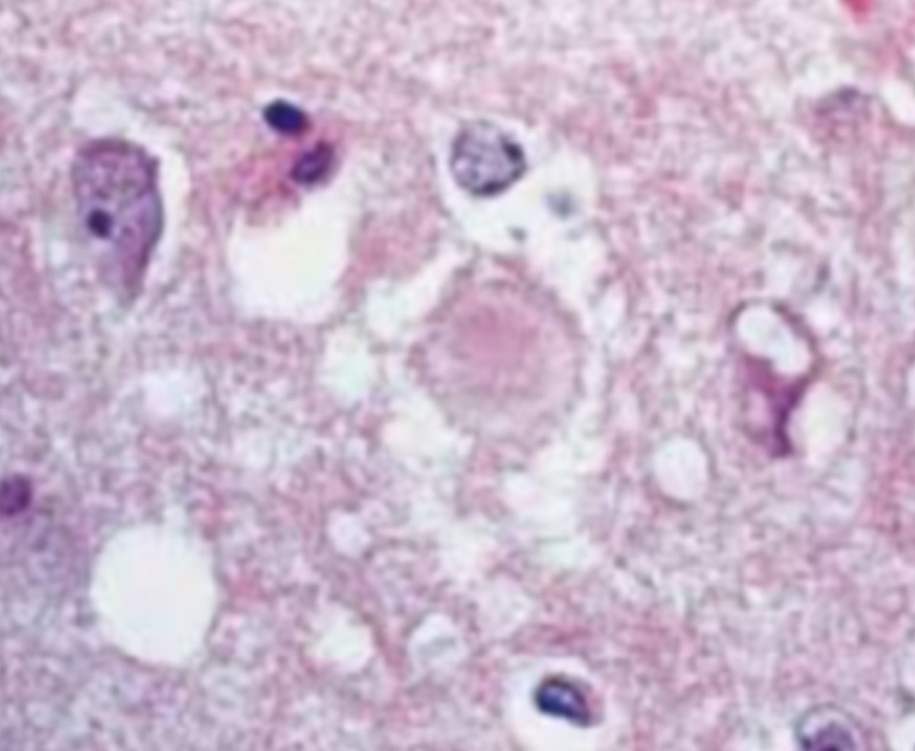

Ref: Outpatient Surgery, A Division of AORN 2018
2. Cost Effectiveness
With the introduction of single use medical devices, concerns have been raised with regards to the increase in costs compared to reusables.
- The use of single use devices removes the need for re-processing and repairs. It also eliminates the risk of cross-infection from a reusable device.
- Reusable devices have an environmental impact with the use of detergents and steam used in processing.
- Several studies have carried out systematic review of the cost effectiveness analysis of reusable versus single devices and have concluded that there are financial benefits from the use of single use devices.
Anaesthesia (2019) A Review Article: A systematic review and cost effectiveness analysis of reusable vs. Single-use flexible bronchoscopes. Mouritsen et al.
3. Save Time
The use of single use instruments saves time as instruments do not have to be reprocessed. This means that planned surgery is not curtailed because reprocessed instruments have not been turned around in time.
Clonallon worked with a Dental Hospital who were experiencing on-going problems in getting the instruments used in a morning clinic reprocessed and turned around for the afternoon clinic.
Switching to single use instruments meant that a full clinic could be run in the afternoon. Additionally, as single use instruments have not been subject to wear and tear it means that replacing a functioning instrument is not required.
4. Environmental Impact
The re-processing of reusable medical devices involves the use of detergents many of which contain phosphates which are known for causing algae blooms when discharged into water courses. Chemical disinfectants are also used in the reprocessing of devices. The use of steam under pressure is commonly used to sterilise chemically cleaned devices and this steam is cooled and discharged as hot water into waste treatment units causing thermal pollution.
A comparative study on environmental impact of reusable and single-use Bronchoscopes using a simplified life-cycle-assessment methodology concluded that there was a higher environmental impact reprocessing a medical device after a second reprocessing event.
